Pain is not a single issue to solve, it is a complex experience that covers physiology, psychology, setting, and assumptions. Effective clinicians discover to read more than a pain rating. They examine the trajectory of discomfort, the threats of undertreatment and overtreatment, the context of the event, and the social Visit this site characteristics that form a patient's action. The expertise system PUAEME008 Offer pain monitoring rests directly in that reality. It is made for initial responders and medical professionals who handle pain in dynamic settings, consisting of prehospital and emergency treatment. One of the most efficient method to provide it, and comparable pain administration courses, is via blended understanding that integrates eLearning, simulation, and office coaching.
I have actually enjoyed talented medical professionals stumble due to the fact that they could recite pharmacology but struggled to titrate analgesia while transporting a person down a narrow staircase at twelve o'clock at night. I have actually also seen peaceful junior nurses outperform positive elders by following a self-displined assessment regimen and by utilizing low-tech procedures that numerous forget. Great training develops both kinds of capacity: knowledge that sticks and tranquil issue solving under pressure.
Where PUAEME008 Fits in the Treatment Landscape
PUAEME008 Give discomfort management (usually reduced to PUAEME008) is frequently consisted of in emergency situation treatment skill sets in Australia and in organisations that mirror that proficiency framework. The device concentrates on examining discomfort, applying ideal discomfort alleviation, monitoring, and documenting results. It anticipates students to operate within clinical governance, follow medication safety concepts, and handle damaging effects.
A common false impression is that this unit is almost medication methods. It is wider. The intent is to make sure a responder can provide pain management that is safe, moral, and reliable for the scenario in front of them. That may mean titrated opioids with capnography, or it could suggest reassurance and splinting while you await back-up. One of the most qualified grads are at ease along that spectrum.
Typical individuals consist of paramedics, event paramedics, nurses in severe setups, physiotherapists that operate in urgent triage or post-operative pathways, and remote clinicians who often work as the very first and only responder. The unit pairs well with resuscitation and trauma modules, yet it additionally strengthens everyday technique in wards and neighborhood care by honing assessment and communication.
Why Blended Understanding Issues for Pain Management Courses
Pain monitoring training programs fail when they lean too heavily on slides and concept. Alternatively, pure simulation without grounding forthcoming causes folklore and irregular care. Blended discovering resolves this by sequencing expertise, practice, and feedback.
An excellent program positions the conceptual heavy training into self-paced eLearning. Learners can absorb neurophysiology, pharmacology, and standards without the time stress of a classroom. After that, the face-to-face part focuses on scenario method, choice making, and the hands-on skills that can not be learned from a screen. Ultimately, monitored workplace application and mentoring locks in routines and gives context that no laboratory can totally replicate.
When you mix PUAEME008 with various other discomfort monitoring training courses, you can map fundamental elements across self-controls while maintaining role-specific proficiencies. Nurses might drill postoperative discomfort plans, while physiotherapists focus on mobilization techniques layered with analgesia timing. Paramedics service multimodal emergency situation pain monitoring in noisy, uncertain atmospheres. Every person shares a typical assessment language and safety and security framework.
Building Blocks: Core Ideas Every Training Course Ought To Cover
Any reliable discomfort management program, whether it causes a discomfort monitoring certificate or stands as one of several brief training courses in pain monitoring, needs to hit a set of non-negotiable concepts.
Start with discomfort systems. Nociceptive, neuropathic, and nociplastic discomfort act in different ways. If a patient with radicular pain at L5 is treated like an ankle joint strain, dissatisfaction is inevitable. Learners should have the ability to recognize warnings, identify peripheral from main sensitization, and recognise when pain is out of proportion to injury.
Assessment is the following column. Numeric ranges are valuable, yet they are not an endpoint. View the breathing pattern, seek sweat, note protective posturing, ask about feature and concerns. In children, empirical devices matter. In older adults, cognitive testing aids differentiate ecstasy from distress. Documentation must videotape both measurable actions and qualitative descriptors due to the fact that those guide titration.
Analgesic pharmacology follows analysis, not in the past. Any discomfort administration qualification program have to press past memorizing doses. It ought to educate titration principles, start and duration differences, synergistic techniques, and negative result mitigation. Paracetamol and NSAIDs do important job if they are timed and incorporated properly. Opioids call for watchfulness with respiration and sedation scales. Ketamine belongs when opioid escalation stalls, particularly in injury, but it brings dissociation and calls for clear approval when possible and structured monitoring. Entonox works and fast for short treatments yet needs testing for caught gas threats. Local anaesthetic methods are effective when within range and competency.
Non-pharmacological strategies are more than home window dressing. Ice, immobilisation, elevation, splinting, comfortable positioning, taking a breath training, diversion, and restorative reassurance reduce analgesic demands. In emergency situation discomfort management, aligning these essentials rapidly changes the trajectory. If you splint correctly and position the limb, the following 10 mins are calmer and more secure for titration.
Finally, administration and interaction matter. In a busy hallway, it is easy to miss identification checks and allergy confirmation. The training ought to apply the discipline of the five rights of medicine, end tidal CO2 tracking where offered, and clear handover: what you gave, when, exactly how the client responded, and what you plan next.
What PUAEME008 Resembles in Practice
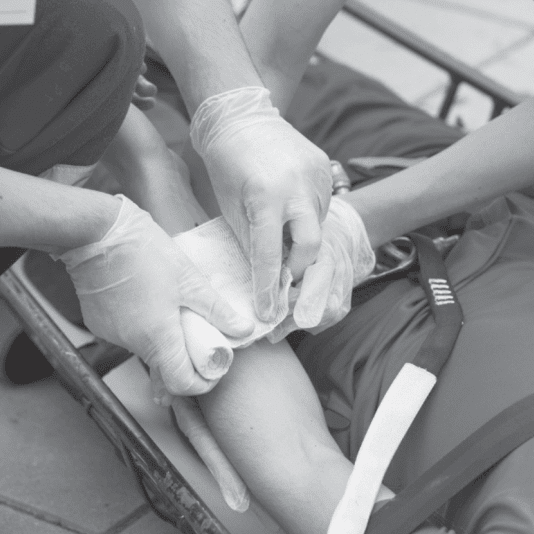
On a wet weekend at a sporting activities ground, a 32-year-old athlete drops awkwardly and presents with apparent forearm deformity. While your companion prepares the splint, you secure the arm or leg, apply cold packs, and begin an organized assessment. Pain at rest is 8 out of 10, even worse with movement. You pre-oxygenate briefly for Extra resources Entonox, check contraindications, and after that coach the patient on self-administered breathing while the splint takes place. The score goes down to 4 out of 10 after five mins, enough to package the patient securely. During transport, you reassess. The inhaled analgesia has actually diminished somewhat, so you give an oral NSAID if not contraindicated and prepare for IV gain access to at the health center for more management.
Different situation. An older grownup with a hip fracture lies in a narrow hallway on the 2nd flooring. The staircases are limited. You offer reduced dose IV fentanyl in tiny increments, seeing respiratory rate and sedation. You position the leg with gentle traction and pillows, then test motion. The client's face stress softens. You pause and observe for 2 minutes before determining whether to give extra. People want another dose swiftly, however persistence keeps you from going after short-term spikes and risking hypoventilation throughout the bring down.
Now a youngster with a partial density burn to the forearm. The moms and dad fears and the youngster is hyperventilating. You prioritise trendy running water for the burn, then topical analgesia where appropriate, and distraction. Ketamine may be thought about for debridement later on, but for transportation the goals are convenience and depend on. PUAEME008 encourages matching the strategy to patient and setting, as opposed to compeling a drug-centric solution every time.
Designing a Blended PUAEME008 Provide Pain Monitoring Course
An efficient provide discomfort management course that maps to PUAEME008 uses a split design and clear assessment standards. Beginning with eLearning modules that require interaction, not just click-through slides. Learners should complete case-based quizzes that branch based upon options, with instant feedback linked to evidence and guidelines. Assign 4 to 6 hours for the on-line section if the system is stand-alone, a lot more if it is packed with airway or injury care.
The face-to-face workshop functions best at 1 day for loan consolidation, or 1.5 days if your associate has vast variation in experience. Keep lecture time tight. Use micro-briefings of 10 to 15 mins, after that revolve with scenarios. Include a minimum of one paediatric situation, one older grown-up, one procedural pain case, and one scenario where analgesia is contraindicated or needs caution. Embed problems: moderate desaturation after opioid titration, introduction responses with ketamine, agitation in a nervous client, or Entonox unavailable at a remote site.
Assessment should be observed, structured, and fair. Use checklists that compensate excellent clinical judgment, not rote recounting. For instance, rather than awarding factors for quoting a standard dose, award points for computing a weight-based dose appropriately, discussing the rationale, and keeping an eye on suitably. Include a recorded pain management plan with review intervals and rise or de-escalation triggers.
Finally, develop work environment application right into the strategy. Learners must finish a log of 3 to 5 genuine cases, de-identified, with short reflections on what altered after training. A trainer or senior clinician can authorize off with comments. This closes the loophole from class to clinical reality.
Tailoring for Different Disciplines
Pain monitoring courses for nurses commonly need to cover post-surgical paths, PCA pump safety and security, opioid-sparing regimens, and discharge education and learning. Emphasise sychronisation with medical prescribers, early warning standards for oversedation, and methods to guide people through the first two days after discharge. Nurses are distinctly positioned to stabilize analgesia with mobilisation, digestive tract treatment, and nausea prevention.
Pain management courses for physio therapists must incorporate analgesia timing with functional goals. A 20 minute window after oral analgesia can be the distinction between safeguarded activity and reliable gait retraining. Show physios to acknowledge when pain is safety and when it has actually come to be maladaptive, and exactly how to coach rated exposure. Include components on communication methods that decrease risk understanding and pain catastrophising, which subsequently decreases analgesic reliance.
Prehospital and occasion clinicians require focused emergency discomfort management with usefulness: bring constraints, oxygen accessibility, environmental obstacles, and single-operator problem fixing. Instruct them to construct a psychological design of the pain gradually. The initial analysis at the scene is frequently unreliable. A 2nd analysis after fundamental actions can avoid overtreatment.
Multimodal Analgesia Without Guesswork
Multimodal techniques are not simply buzzwords. They help by striking discomfort along different pathways and by smoothing the peaks and troughs that bring about dosage piling. An usual error is to include numerous agents from the exact same class, or to time them in such a way that hides negative impacts up until they collide.

Think in layers. Beginning with paracetamol otherwise contraindicated, then include NSAIDs where safe, and layer an opioid only if discomfort stays considerable or if the mechanism suggests that non-opioids will certainly underperform. For stressful bone and joint pain, regional techniques by qualified clinicians can be decisive. For neuropathic functions, early acknowledgment stops chasing greater opioid doses and unlocks to complements and education.
Another layer is environmental and emotional. Discuss what you are doing and why. Patients that feel regulated and educated often need much less drug. That is not sugar pill, it is physiology and count on working together. For some, the ideal words at the best time are as impactful as an additional 25 micrograms of fentanyl.
Safety Nets: Surveillance and Escalation
Safety is not a checklist you tick as soon as. It is a loop. Prior to you carry out, you verify identity, allergic reactions, standard vitals, and threat aspects. While providing, you titrate to effect with repaired review points. Later, you keep track of and determine whether to rise, maintain, or back off.
For opioids, utilize unbiased sedation ranges and respiratory rate, and when available, end tidal carbon dioxide. A decrease in respiratory rate is late. Increasing carbon dioxide can caution you previously. Have reversal agents and a prepare for assisted air flow. For ketamine, plan for introduction reactions. A tranquil setting, a clear explanation, and a small benzodiazepine dosage in particular protocols can minimize that danger. For Entonox, screen for bowel obstruction, pneumothorax danger, or recent diving.
Documentation is an additional safety tool. When you tape-record timing, dosage, route, and reaction, you minimize the chance of increasing up and you develop a narrative that helps the next clinician. The discomfort management certificate several organisations problem is only like the practices it reflects. Habits stay in documentation and handover as much as they stay in your fingers.
Short Training courses hurting Administration: What Works and What to Avoid
Short programs in pain management can enhance certain skills quickly, but they should not oversell. A two-hour workshop can develop your splinting and breathed in analgesia workflow, but it will not transform your strategy to complex neuropathic discomfort. Pick a training course that explicitly specifies its extent and assessment method.
Some programs promise a pain administration certification in a weekend break with heavy focus on unique techniques. Beware of glossy material that ignores basic analysis. If participants leave without a solid understanding of red flags, contraindications, and informed permission, the course is not serving them. Try to find programs that consist of follow-up touchpoints, such as instance examines at 4 to 6 weeks. Those reinforce modification and keep the knowing honest.
What to Expect From a Top Quality Pain Management Certification Course
When a carrier advertises a discomfort administration qualification training course, see the certification as the endpoint of a series, not a memento. Solid programs reveal you an educational program map, teacher credentials, governance policies, and a plan for remediation if you do not fulfill conventional. They incorporate PUAEME008 Offer pain management or comparable requirements where appropriate, and they analyze with circumstances that resemble your work, not abstract cases.
The much better programs also instruct you just how to measure end results. That may suggest tracking a division's typical time to initial analgesia, the percentage of individuals with recorded review within 15 minutes, or the price of opioid dose decreases in the very first 1 day after surgical procedure. These are not vanity metrics. They point to behavior modifications that reduce harm and boost comfort.

Training for Teams, Not Just Individuals
Pain administration training for registered nurses, physiotherapists, and very first -responders has the best influence when groups educate with each other. Shared language minimizes rubbing. If the registered nurse and paramedic both utilize the same sedation range and the same review schedule, handovers are cleaner and errors decline. Group situations likewise reveal process snags. I when viewed a team uncover that their Entonox was stored in a secured cabinet on a different flooring than their splinting set. After a single drill, they relocated both to the same cart and cut minutes off their response.
Teams likewise enhance uniformity in patient messaging. When every person discusses the plan with the exact same expressions, individuals feel connection. That decreases anxiousness and helps you utilize less medicines to attain much better comfort.
Common Challenges and Exactly how to Avoid Them
Several errors repeat throughout services and settings. Overreliance on a single agent leads to dose stacking. Provide the medicine time to function, watch, then act. Underuse of non-pharmacological procedures is an additional. A well-fitted splint and a calm area can spare a second opioid dose.
Documentation drift is a chronic problem. Busy changes wear down excellent habits. Use pocket triggers or electronic chart layouts that force a reassessment area. Advise associates that what is not composed ends up being unnoticeable at the following handover.
Scope creep can happen after certification. Someone discovers a new strategy, feels great, and starts utilizing it in side situations without assistance. Excellent administration collections boundaries and provides pathways to extensive expertises with supervised technique, not ad hoc experimentation.
Crafting Your Course: Picking the Right Discomfort Administration Educating Courses
Choose based upon your function, your common person accounts, and your solution restraints. If you work event medicine with restricted tools, prioritise a PUAEME008-aligned workshop with solid simulation and transport situations. If you are a ward registered nurse, look for a discomfort management certification training course that incorporates PCA security, opioid-sparing strategies, and discharge preparation. Physio therapists should look for programs that link analgesia timing and graded movement, with material on interaction to decrease fear-avoidance.
Ask providers tough concerns. Who shows the course and what is their present professional practice? Just how will they analyze you? What post-course assistance is consisted of? Just how is the discomfort monitoring certification confirmed? Do they map to recognised systems like PUAEME008 Give pain management? Answers to these concerns predict training course value better than shiny brochures.
A Practical Structure You Can Make Use Of Tomorrow
Here is a small framework that supports risk-free, reliable care throughout settings.
- Assess extensively: system, red flags, baseline vitals, pain descriptors, feature impact, psychosocial factors. Act in layers: non-pharmacological actions first, then pharmacological agents timed and titrated, with multimodal combinations. Reassess deliberately: establish a timer, check discomfort, function, sedation, respiration, and make a decision to intensify, maintain, or de-escalate. Communicate and record: share the strategy, capture dose-response timing, turn over clearly. Reflect and change: capture a brief case note later, determine what functioned and what to improve.
This is not a technique. It is a structure that turns mayhem right into manageable actions. Follow it constantly, and your outcomes boost steadily without heroics.
The Worth of Accreditation When It Is Done Right
A pain administration certification confirms that you satisfied a requirement on a specific day. Its real value remains in the habits it cements and the confidence it earns from your peers and patients. When you complete a certificate training course in pain management that consists of PUAEME008 Provide discomfort monitoring or its comparable, you are registering for a way of working: disciplined analysis, gauged treatment, thoughtful rise, and precise handover.
Organisations that invest in discomfort monitoring training programs with mixed distribution see tangible gains. Less people wait greater than 20 mins for very first analgesia. Fewer experience oversedation. Personnel report extra confidence in addressing complex pain without reflexively grabbing greater dosages. Those outcomes are not instant, yet they build up as personnel repeat the self-control day after day.
The best part is that this strategy ranges. It aids in a noisy hallway, on a cot in the rain, in a post-op bay at 3 a.m., and in the silent conversation prior to a client takes their first steps after surgical treatment. Mixed learning, secured by durable devices like PUAEME008, turns discomfort management from a collection of methods into an incorporated medical craft.